The ‘drama’ — the seemingly magical disappearance of pain — that occurred in the body of the surgeon-patient of the previous post on placebo, requires two separate ‘dramatic’ acts:
1) anticipation of relief, preceding
2) the experience of it.
Act 1: Anticipation or expectation of relief
The “stars” of Act 1 are the surgeon’s prefrontal cortex (PFC),
 which orchestrates thoughts and actions in accordance with internal goals, and the Anterior Cingulate Cortex (ACC)
which orchestrates thoughts and actions in accordance with internal goals, and the Anterior Cingulate Cortex (ACC)
 which is involved in processing emotion and motivation. [2][17][15][27]. The saline-induced relief from pain would not have occurred if there had not first been increased activity in these two locations due to the anticipation of relief from pain.
which is involved in processing emotion and motivation. [2][17][15][27]. The saline-induced relief from pain would not have occurred if there had not first been increased activity in these two locations due to the anticipation of relief from pain.
The surgeon’s body was not responding to the essentially empty injection, so much as responding to his desperate-for-relief belief that the injection was morphine, a belief which begins with activity in the PreFrontal Cortex and the Anterior Cingulate Cortex.
Once the two locations ‘decide’ (in a very loose sense) that the injection is the real thing (i.e., morphine), they set into motion biochemical pathways

The opioid system
of endogenous (‘self-made’) opioids that activate painkilling pathways very similar to the pathways activated by the ‘real’ drug. That’s why pain ‘treatments’ that are essentially just sugar or water can result in the lessening of pain. The placebo treatment looks identical enough to the ‘active’ treatment to create an expectation (assumption, anticipation) that it will have the same effect that the ‘active’ drug is reputed to have. The rest of the brain then responds to that expectation, triggering biochemical changes a the site of pain in the body, via nerves that lead from the brain through the spinal cord to the site.
Thus, most commercial drugs owe at least some degree of their success to a placebo response which is induced by belief in the drug[13]. To get an idea of which drugs have a placebo component and which don’t, search ‘clinical trial’ thenameofthedrug ‘placebo’ and look for a statement which says something like “X percent responded to the drug, whereas only Y percent [usually a smaller percent] responded to placebo.” If it says “0% responded to placebo”, then the drug has no placebo component. Otherwise, the body’s innate self-healing placebo response is at least part of that drug’s ability to do what it does.
Not surprisingly, researchers have found as well that people who respond poorly to a placebo also tend to respond poorly to the ‘active’ treatment [15][17]. Thus, it’s a misnomer to use the terms ‘active treatment’ versus ‘placebo treatment’: both treatments are ‘active’, and both are at least part ‘placebo’.

Responder to BOTH placebo and 'active' treatments

OR, a responder to NEITHER placebo nor 'active' treatments
Responders to placebos and to traditional drugs appear to have the capability to summon up the biochemical pathways that underlie, at a minimum, the placebo response. Note: The existence of a placebo that works like a traditional treatment is not true for all diseases. The neural pathways involved in placebo have so far been studied extensively only for pain, depression, and Parkinson’s disease.
(Why not placebos for all diseases? )
But in terms of killing pain, responders to both active and placebo components of a treatment must, at a minimum, have functioning opioid pathways [15].

The opioid system
Act 2: the Experience of relief
Just as the PreFrontal Cortex and rostral Anterior Cingulate Cortex perform the act of anticipation/expectation , so do the pain-processing areas of the brain (the thalamus
 ,
,
the insula

and the caudal (rear) ACC
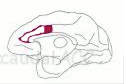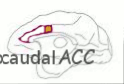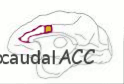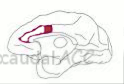
) take on, in the second act, the experience of pain relief. The biggest changes overall between anticipation of pain relief and the actual experience of it is that there is increased activity during anticipation in the structures responsible for the anticipation of relief, and decreased activity when pain lessens, in the structures responsible for the experience of relief.
(If the thalamus is insensitive to pain, why would it be involved? )
Figure 1 below shows the structures involved both in pain that is untreated (in the top half) as well as the structures affected by opioids (bottom left) and by placebos (bottom right).

Fig.1 from Petrovic et al. 2002(ref.15)
Expectation induced by a placebo for morphine (and for some other medicines) registers in the PreFrontal Cortex
and has the end result of stimulating opioids which the body produces naturally (i.e., endogenous opioids) [20] [17]. Consider this: the chemical naloxone , when given as a injection, is known to block the painkilling effect of opioids, including morphine. What’s amazing and yet entirely logical is that it also blocks the painkilling effect of a placebo, even in someone previously established as a placebo responder. [20] [15] [14] [22] [23] That’s because morphine and a morphine-look-alike placebo (which stimlates endogenous opioids) engender very similar biochemical changes in response to pain — changes that start in the brain and cascade from there. And thus both are blocked in similar ways by the same chemical (naloxone).
Indeed, and who would ever have thunk: An endogenous opioidlike material has been found in the cerebrospinal fluid

Removing fluid from the spinal column
of chronic pain patients whose pain level dropped following placebo administration [14].
References
2. Leuchter F et. al.: changes in brain function of depressed subjects during treatment with placebo. Am J Psychiatry 2002; 122-129
13. Kirsch I, Sapirstein G: Listening to Prozac but hearing placebo : A meta-analysis of antidepressant medication. Prevention and Treatment 1998; 1(0002a)
14. Fields HL, Price DD: Toward a neurobiology of placebo analgesia, in The Placebo Effect: An Interdisciplinary Exploration. Edited by Harrington A. Cambridge, Mass., Harvard University Press, 1997 p.93-116
15. Petrovic P et. al.: Placebo and opioid analgesia – imaging a shared neuronal network. Science 2002; 295(5560): 1737-1740
17. Wager TD et. al.: Placebo-induced changes in fMRI in the anticipation and experience of pain. Science 2004; 303(5661): 1162
20. Amanzio M, Benedetti F: Neuropharmacological dissection of placebo analgesia: expectation-activated opioid systems versus conditioning-activated systems. Journal of Neuroscience 1997; 19(1): 484-494
22. Benedetti F et. al.: Somatotopic activation of opioid system s by target-directed expectations of analgesia. Journal of Neuroscience 1999; 19(9): 3639-3648
23. Johansen O, et. al.: Placebo and Nocebo Responses, cortisol, and circulating beta-endorphin. Psychosomatic Medicine 2003; 65: 786-790
27. de la Fuente-Fernandez et. al.: Placebo mechanisms and reward circuitry; clues from Parkinson’s disease. Biological Psychiatry, 2004.
This page has the following sub pages.
[…] How could a placebo for a painkiller actually kill pain? […]